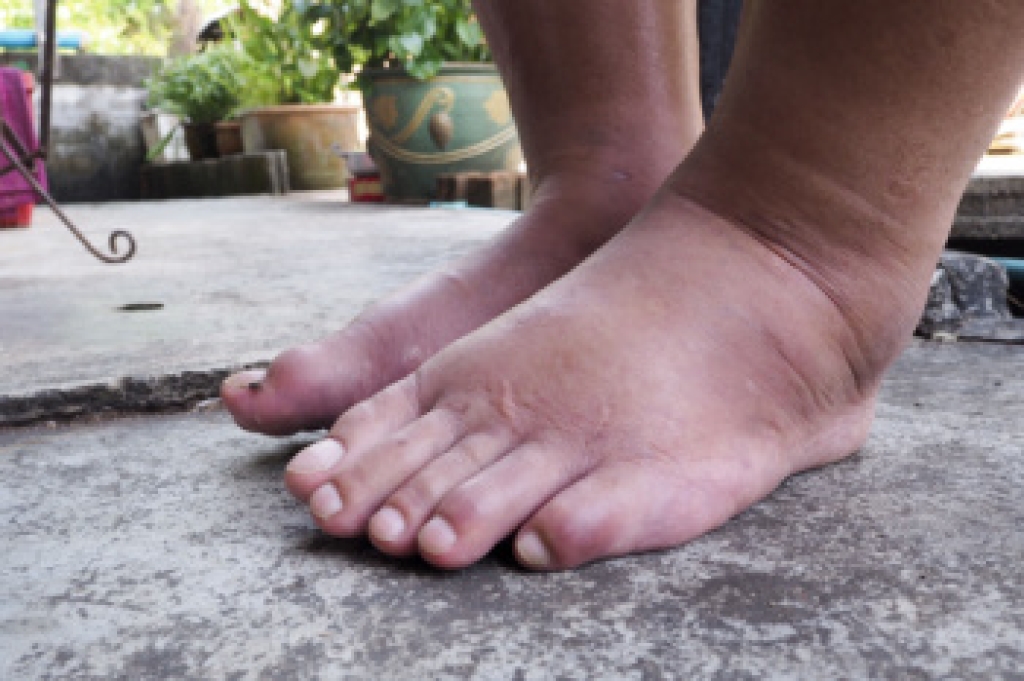
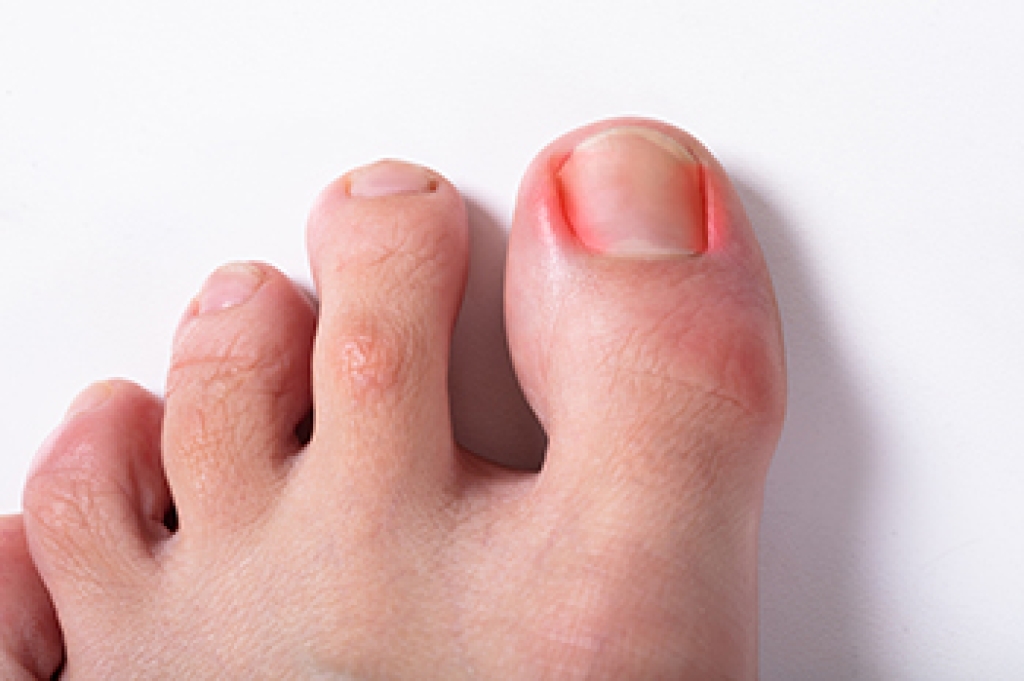
Pain in the ball of the foot, termed metatarsalgia, refers to discomfort under the front part of the foot where weight is placed when walking. This pain can feel like a dull ache or a burning sensation, and it may worsen with standing or activity. Common causes include overuse, foot injuries, and pressure from wearing tight or high-heeled shoes. Conditions like a thickened nerve, joint strain, or a small fracture may also contribute to symptoms. Some people notice tingling or numbness in the toes, which can point to nerve involvement. Risk factors include aging and high-impact activities. Poor foot alignment can also increase stress in this area. A podiatrist can evaluate the foot and use imaging to identify the source of pain. Treatment includes custom orthotics, padding, footwear guidance, or other methods to reduce pressure and improve function. If you have pain in the ball of the foot, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Jordan Baker, DPM from Best Foot Forward Surgical Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Florence, SC . We offer the newest diagnostic and treatment technologies for all your foot care needs.